
At the office of Plaza Dental Parker, we prioritize thoughtful decision-making and patient comfort when extractions become part of a treatment plan. Removing a tooth is never the first choice — our clinicians explore every reasonable option to preserve natural teeth — but extraction is sometimes the safest, most predictable step to protect oral health and prevent future complications.
Decisions about extractions are based on a careful evaluation of your dental and medical history, clinical examination, and imaging. We’ll explain the reasons behind our recommendation, outline any alternatives that may be appropriate, and describe what to expect before, during, and after the procedure so you can make an informed choice.
For many patients, an extraction resolves pain, removes a source of infection, or creates space needed for proper alignment. Throughout the process, our goal is to minimize anxiety and discomfort while focusing on efficient healing and long-term oral stability.
Primary (baby) teeth that do not fall out on schedule
Sometimes a primary tooth remains firmly attached and blocks the eruption of its permanent successor. When a baby tooth becomes ankylosed (fused to bone) or its roots fail to resorb, removal can help the permanent tooth come in correctly and prevent crowding or misalignment as your child’s mouth develops.
Damage from extensive decay that cannot be restored
When decay progresses beyond the point where a filling or crown can reliably rebuild the tooth, extraction may be the most predictable way to eliminate infection and protect neighboring teeth and tissues. Removing a non-restorable tooth prevents the spread of disease and allows for planning a replacement if needed.
Severe fractures or structural compromise of the tooth
Teeth that are cracked through the root, split vertically, or fractured in a way that jeopardizes long-term function often cannot be salvaged. When repair would be unreliable or could lead to recurrent problems, extraction is considered to preserve overall oral health.
Advanced periodontal disease affecting tooth support
Periodontal disease weakens the bone and soft tissues that hold teeth in place. In advanced cases where mobility is significant and supporting structures cannot be restored predictably, extraction may be necessary to remove a source of ongoing inflammation and prepare the mouth for restorative planning.
Wisdom teeth that are impacted, decayed, or misaligned
Third molars commonly lack space to erupt properly and can cause crowding, infections, or damage to adjacent teeth. When wisdom teeth present a clear risk now or in the near future, removal can prevent painful complications and simplify long-term maintenance.
Extractions as part of orthodontic planning
In some orthodontic cases, removing specific teeth creates the space needed to align the remaining teeth and achieve a balanced, functional bite. Extractions for orthodontic reasons are carefully planned and coordinated with your orthodontist to support the overall treatment goals.
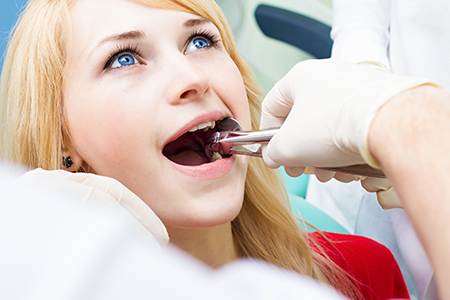
Before any extraction, we conduct a comprehensive review that includes your medical history, a dental exam, and appropriate imaging. Digital radiographs help our team understand root shape, the proximity of nearby structures, and whether the tooth is likely to come out easily or require a more involved approach.
Knowing your medical background and current medications is essential. Certain health conditions or drugs can influence healing or increase risk, so we’ll determine whether any additional precautions are necessary, such as antibiotic coverage, medication adjustments, or coordination with your physician.
We’ll also discuss anesthesia and comfort options. Most extractions are completed under local anesthesia, and for patients who require extra support we provide dental sedation options to reduce anxiety and improve the overall experience.
A simple extraction is performed when the tooth is visible in the mouth and has a straightforward root form. After numbing the area with a local anesthetic, the clinician gently loosens the tooth and removes it with forceps. The procedure is typically quick, and we’ll provide instructions to manage bleeding and discomfort immediately afterward.
When a tooth is broken below the gumline, impacted, or fused to bone, a surgical approach is required. This involves making a small incision in the gum and, if necessary, removing a small amount of bone to access and section the tooth for safe removal. Surgical extractions are performed with precise technique to protect adjacent tissues and promote predictable healing; some cases are referred to an oral surgeon when appropriate.
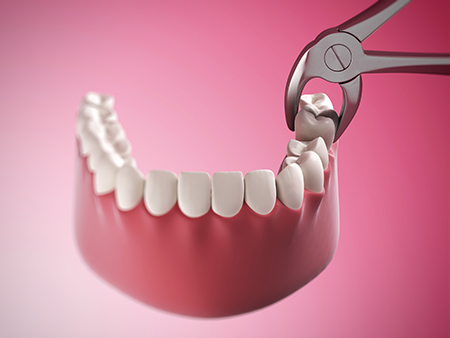
Recovery after an extraction varies by the complexity of the procedure and your individual health. Most patients experience manageable soreness and mild swelling for a few days. Following the post-operative guidelines we provide helps reduce pain, prevent complications, and support healthy tissue repair.
We’ll recommend a timeline for when to resume normal activities and when to schedule a follow-up visit if one is needed. If a tooth is being replaced later with an implant, bridge, or denture, removal is planned with those restorative steps in mind so you have a clear path forward.
If you notice persistent heavy bleeding, severe pain that does not respond to medication, or signs of infection such as fever or spreading swelling, contact the office so we can evaluate you promptly.
Control bleeding with gentle pressure
After the procedure you will be given gauze to bite on. Maintain firm, steady pressure for the first hour and replace the gauze as instructed. Light oozing can continue for up to 24 hours, but prolonged or heavy bleeding should be reported to the office.
Protect numb tissues
Avoid chewing, touching, or probing the area until anesthesia wears off to prevent accidental biting of lips, cheeks, or tongue.
Follow medication guidance
Take any prescribed antibiotics or pain medications exactly as directed. Over-the-counter pain relievers can be effective for most discomfort; take them according to the instructions and any guidance we provide.
Protect the clot
Do not rinse vigorously, spit, use a straw, or smoke during the initial 24–72 hours. These actions can dislodge the clot and lead to delayed healing or a painful condition called dry socket.
Manage swelling and comfort
Applying ice to the face in 10-minute intervals during the first 24 hours helps limit swelling. Rest and limit strenuous activity for the first couple of days to aid recovery.
Choose gentle foods
Stick to soft, cool, or room-temperature foods for the first few days. Avoid hot, spicy, or carbonated beverages until healing is more established, and drink plenty of water.
Keep your mouth clean
Carefully brush your other teeth and, when advised, rinse gently with a warm saltwater solution to maintain hygiene without disturbing the extraction site. Resume your normal oral hygiene routine as recommended by our team.
Attend follow-up appointments
If sutures were placed or additional monitoring is needed, keep the scheduled follow-up so we can confirm proper healing and discuss next steps for restoration if necessary.
If you experience ongoing problems such as increased pain, swelling, a bad taste, or other unusual symptoms, contact our office so we can provide guidance and, if necessary, arrange an evaluation.
When an extraction is the best clinical path, patients look for a team that combines experience, clear communication, and a calm approach to comfort. Our clinicians focus on gentle technique, thorough planning, and individualized care that considers both immediate needs and long-term oral health goals.
We coordinate extractions with restorative planning so that replacing a missing tooth — when appropriate — becomes a predictable, well-timed part of your overall treatment. Whether the next step is a removable prosthesis, a fixed bridge, or a dental implant, we’ll review options and timelines and help you understand what to expect.
Our priority is to guide you through the process with straightforward information, attentive care, and follow-up support so you can move forward with confidence and a clear plan for maintaining or restoring your smile.
A tooth extraction is recommended when preserving the natural tooth is no longer predictable or safe for surrounding tissues. Common reasons include extensive decay that cannot be restored, severe fractures that compromise function, advanced periodontal disease with significant mobility, and impacted or problematic wisdom teeth. Extractions are also planned when a primary tooth blocks the eruption of a permanent tooth or as part of orthodontic treatment to create space.
Decisions about removal are made after a careful clinical exam and appropriate imaging so the risks and benefits are clear. When possible, clinicians will describe alternatives such as endodontic therapy, periodontal treatment, or restorative solutions that may preserve the tooth. The primary goal is to protect oral health and prevent future complications for neighboring teeth and tissues.
When removal is the most predictable option, the treatment is planned to support efficient healing and future restoration when needed. This includes coordinating with the patient on timing and discussing options for replacing the missing tooth if appropriate. Clear information about the reasons for extraction helps patients make informed choices about their care.
The evaluation starts with a comprehensive review of your dental and medical history, a clinical examination, and diagnostic imaging such as digital radiographs. Imaging reveals root anatomy, proximity to important structures, and whether the tooth is likely to come out easily or require a surgical approach. Knowing your medications and health conditions is essential because certain factors can influence healing and increase risk.
During the consultation, the clinician explains the findings and discusses alternatives when appropriate, including the likelihood of success for restorative treatments. We consider your symptoms, overall oral health, and long-term treatment goals when recommending extraction or preservation. Collaboration with specialists or your physician may be arranged if additional evaluation is needed.
Consent and preparation are part of the process so patients understand what to expect before, during, and after the procedure. The team outlines anesthesia options, potential complications, and follow-up plans to promote safe and predictable care. This thorough approach reduces uncertainty and supports informed decision making.
A simple extraction is performed on a tooth that is fully visible in the mouth and has a straightforward root form. After local anesthesia numbs the area, the clinician gently loosens the tooth with elevators and removes it with forceps; the procedure is typically quick and recovery is generally uncomplicated. Simple extractions are common for primary teeth, mobile teeth, or teeth with uncomplicated root anatomy.
Surgical extractions are required when a tooth is broken below the gumline, impacted, or fused to bone, or when root anatomy is complex. The procedure may involve making a small incision in the gum, removing a bit of bone, and sectioning the tooth into pieces for safe removal. Surgical cases are handled with techniques to protect surrounding tissues and promote predictable healing, and some complex cases are referred to an oral surgeon when appropriate.
Whether a simple or surgical approach is needed is determined by the clinical exam and radiographic findings. The team will describe the planned technique and outline post-operative care specific to the type of extraction. Understanding the differences helps patients prepare for recovery and follow-up needs.
Most extractions are performed using local anesthesia to numb the treatment area so the tooth can be removed comfortably. For patients who experience anxiety or require more extensive procedures, additional options such as nitrous oxide (laughing gas), oral conscious sedation, or monitored moderate sedation may be available. The choice of sedation depends on the complexity of the extraction, the patient’s medical history, and personal comfort preferences.
Before recommending sedation, the clinician reviews your medical history, current medications, and any prior experiences with sedation or anesthesia. Certain health conditions or medications may require special precautions or coordination with your physician to ensure safety. When sedation is used, staff monitor vital signs and provide instructions for pre-procedure fasting and post-procedure recovery, including arranging transportation if needed.
At Plaza Dental Parker, the team discusses anesthesia and sedation options during the consultation so you can select the level of comfort that best meets your needs. Clear pre- and post-operative guidance helps ensure a controlled, safe experience regardless of the chosen modality. If a case requires deeper sedation or hospital-based care, a referral is made to an appropriate specialist.
Preparation begins with a detailed discussion of your medical history and current medications, including blood thinners, diabetes medications, and any recent illnesses. Follow any specific instructions provided by the clinic regarding fasting or adjustments to medications if sedation will be used, and bring a list of your medications to the appointment. Arrange transportation home if you will receive sedation that impairs your ability to drive or make important decisions.
On the day of the procedure, wear comfortable clothing and avoid applying strong cosmetics or lip products that could interfere with monitoring equipment. If you smoke, try to refrain before and after the extraction because smoking increases the risk of complications and delays healing. Ask questions about what to expect during recovery and confirm follow-up arrangements before you leave the office.
Having soft foods, ice packs, and any recommended over-the-counter pain relievers on hand can simplify immediate post-operative care. Clear instructions about activity restrictions and clot-protecting behaviors (such as avoiding straws and vigorous rinsing) will be provided. Preparing in advance helps promote a smoother recovery and reduces the chance of unexpected issues.
During the first 72 hours it is normal to experience some bleeding, mild to moderate discomfort, and swelling around the extraction site. You will be instructed to bite gently on gauze to control bleeding and to apply ice to the face intermittently during the first 24 hours to limit swelling. Pain can usually be managed with recommended over-the-counter analgesics or prescribed medications when appropriate, and following dosing instructions is important for comfort.
Protecting the blood clot that forms in the socket is essential to avoid complications such as dry socket; avoid vigorous rinsing, spitting, using a straw, or smoking during the initial 24–72 hours. Stick to soft, cool or room-temperature foods and maintain hydration while avoiding hot or spicy items that can irritate the site. Gentle oral hygiene around the area is encouraged, and you may be advised to begin warm saltwater rinses after the first day to support cleanliness without disturbing healing tissues.
If you notice persistent heavy bleeding, fever, spreading redness or swelling, or severe pain that does not respond to medication, contact the office promptly for evaluation. Most patients progress uneventfully with these precautions, but early communication ensures timely care if problems arise. A follow-up visit may be scheduled to check healing and discuss restorative planning when appropriate.
Dry socket, or alveolar osteitis, occurs when the blood clot in the extraction socket is dislodged or dissolves prematurely, exposing bone and nerve endings and causing significant pain. Symptoms typically begin a few days after the extraction and include a deep, throbbing pain radiating from the site, a bad taste in the mouth, and visible bone in the socket for some patients. Certain factors—such as smoking, poor oral hygiene, traumatic extractions, and use of oral contraceptives—can increase the risk.
Treatment involves an in-office evaluation and gentle management to relieve pain and promote healing; clinicians often place a medicated dressing or dressing that soothes the exposed area and may prescribe analgesics for symptom control. Instructions are given to maintain oral hygiene and avoid behaviors that could further disturb the socket while the tissue heals. With appropriate care, symptoms typically improve over several days and the socket gradually closes.
Prevention focuses on protecting the initial clot by following post-operative instructions carefully, avoiding smoking, and following any activity restrictions. If you develop severe pain after an extraction, contact the dental office so the team can assess the site and initiate appropriate treatment. Timely intervention reduces discomfort and supports a predictable recovery.
The timing for replacing a missing tooth varies based on the extraction complexity, the condition of the surrounding bone, and your overall treatment goals. In some cases, immediate implant placement is possible at the time of extraction, while other situations benefit from a healing period or socket preservation with a bone graft to optimize bone volume. Your clinician will evaluate radiographs and discuss options for immediate, early, or delayed replacement based on predictable esthetic and functional outcomes.
Common restorative options include dental implants, fixed bridges, and removable prostheses, each with specific timing considerations related to healing and tissue stability. Coordination between the surgical and restorative phases ensures that replacement choices are planned to achieve long-term success. The team will explain the advantages and clinical requirements of each option so you can make an informed decision about the next steps.
Follow-up appointments are used to monitor healing and schedule the appropriate phase of restorative care when ready. If additional procedures such as bone grafting or ridge preservation are recommended, these are incorporated into the timeline to support optimal implant or prosthetic placement. A clear plan helps patients understand how extraction fits into their broader treatment pathway.
Medical conditions such as diabetes, bleeding disorders, cardiovascular disease, and certain bone medications (for example, bisphosphonates) can affect healing and risk associated with dental extractions. Likewise, medications like anticoagulants and antiplatelet agents influence bleeding control and require careful coordination with your prescribing physician. Providing a complete medical history and current medication list allows the dental team to tailor the extraction plan and determine whether any pre-procedure adjustments or consultations are necessary.
For patients on blood thinners, the clinician will assess bleeding risk and may communicate with the medical provider about temporary adjustments when indicated. Antibiotic coverage or specific post-operative precautions may be recommended for patients with particular medical conditions or prosthetic devices. Safety is prioritized by following evidence-based protocols and collaborating with other healthcare providers as needed.
Open communication about your health and medications before the procedure reduces the chance of surprises and helps ensure a controlled approach to care. If you have concerns related to a chronic condition or recent medical changes, mention them during your consultation so the team can make appropriate preparations. Proper planning supports safe treatment and predictable healing.
Plaza Dental Parker provides coordinated care that emphasizes clear communication, careful planning, and attention to comfort during extractions. The team conducts thorough evaluations, uses digital imaging to guide treatment decisions, and discusses anesthesia and sedation options when appropriate to meet individual needs. When extractions are part of a broader restoration plan, the clinicians align surgical and prosthetic steps to support predictable long-term outcomes.
The office accommodates same-day appointments for dental emergencies and works to reduce anxiety for patients who are nervous about treatment by offering appropriate sedation alternatives and supportive care. Clinicians refer complex surgical cases to specialists when that pathway best serves the patient’s safety and prognosis. Follow-up and clear post-operative instructions are provided to support healing and address any concerns promptly.
Choosing a practice that prioritizes patient education and interdisciplinary planning helps ensure you understand each step of the process and what to expect during recovery. If you have questions about extractions or need an evaluation, the team at Plaza Dental Parker can review your situation, explain options, and coordinate the appropriate care pathway.
