When a tooth is lost, the effects go beyond a gap in your smile. Missing teeth can change how you chew, how your bite functions, and over time they can accelerate wear and shifting of neighboring teeth. Dental implants address these issues by replacing both the visible crown and the underlying support structure, which helps preserve jaw alignment and overall oral health.
Implants are composed of biocompatible materials designed to integrate with bone, creating a stable foundation for a crown, bridge, or denture. Their design restores chewing efficiency and speech and often feels far more natural to patients than removable options. Because they fuse with the jaw, implants also help maintain the facial contours that can be lost after tooth extraction.
Many patients choose implants because they offer a durable, long-term outcome that supports everyday life—eating, speaking, and smiling—without the concerns that come with removable prostheses. If you’re evaluating tooth replacement options, understanding what implants can deliver is a helpful first step toward a confident, functional smile.

A dental implant begins as a small, sturdy post surgically placed into the jawbone. Over a period of healing, the bone grows around the implant in a process called osseointegration. This creates a strong mechanical bond that mimics the function of a natural tooth root and provides a stable anchor for a final prosthetic restoration.
Treatment begins with careful planning, including a detailed review of your medical and dental history and imaging to assess bone volume and anatomy. That preparation lets the dental team determine the ideal implant position and prosthetic design, so the final restoration looks natural and performs reliably. Many patients appreciate the step-by-step nature of the process: evaluation, placement, healing, and final restoration.
Surgery to place an implant is typically performed in an outpatient setting and is often well tolerated. Our team discusses anesthesia and sedation options beforehand and provides clear pre- and post-op instructions. Following placement, a short healing period is needed for stability before the permanent crown or prosthesis is attached, though in select cases a temporary restoration may be placed immediately.
One of the most compelling advantages of dental implants is their ability to restore both form and function. Because an implant replicates the root structure, it supports chewing forces much like a natural tooth and reduces the risk of movement or slippage that can occur with removable dentures. That reliability makes meals and conversation more comfortable and predictable.
Implants also help preserve the jawbone. When a tooth is missing, the underlying bone can begin to resorb over time; placing an implant provides the stimulation the bone needs to retain its volume and strength. This preservation helps maintain natural facial contours and supports the long-term health of adjacent teeth.
With proper care—regular hygiene and routine dental visits—implants can last for many years and often for decades. They are resistant to decay and, because they do not rely on neighboring teeth for support, can be a conservative solution compared with traditional bridgework. For many patients, that combination of durability, function, and bone preservation makes implants the preferred option.
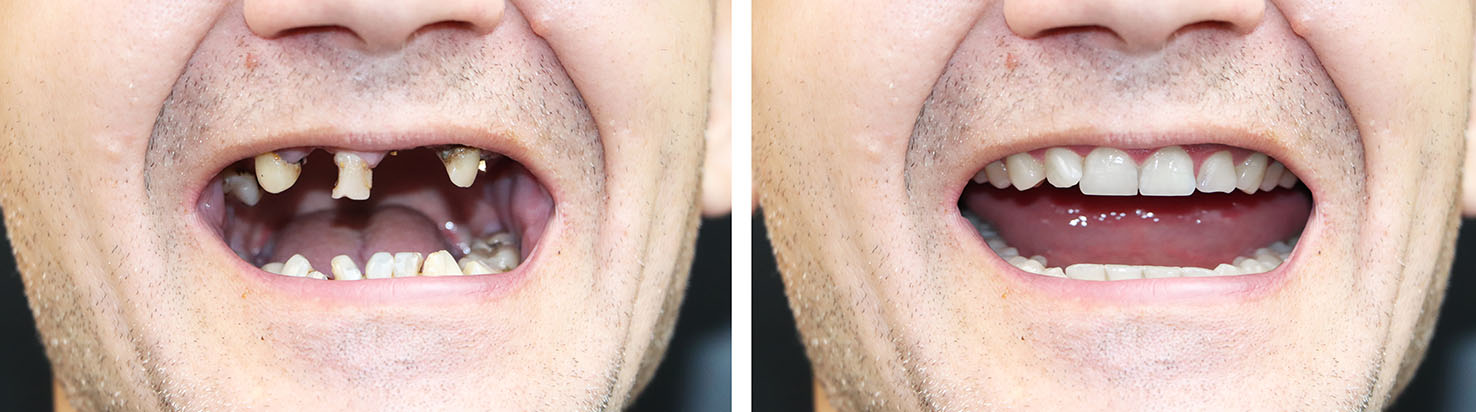
Implant dentistry is flexible: a single implant with a crown replaces an isolated missing tooth, while multiple implants can support bridges or full-arch prostheses. The right plan depends on how many teeth are missing, the condition of the supporting bone, and your personal goals for function and aesthetics.
For patients missing one tooth, a single-tooth implant and crown restore the area without altering adjacent healthy teeth. When several teeth are missing in a row, implant-supported bridges can replace them without relying on surrounding teeth for support. For complete arches, a limited number of implants can anchor a fixed bridge or provide retention for an overdenture, improving comfort and function compared with conventional dentures.
Because the approach is tailored, each solution balances simplicity, durability, and the patient’s expectations. Your dental team will outline the available options, describe the expected timeline for healing and restoration, and recommend the plan that best matches your oral health and lifestyle.
Determining candidacy for implants involves a thoughtful review of your overall health, dental history, and specific oral conditions. Important considerations include the quality and quantity of the jawbone, the presence of gum disease, and any medical conditions that might affect healing. Age alone is rarely a limiting factor; the primary focus is on health and suitability for surgery.
Imaging and clinical measurements give the team a clear picture of bone levels and anatomy so they can plan implant placement precisely. If bone is insufficient in an area, a grafting procedure can rebuild volume to support an implant. The intent is to create predictable, stable results while minimizing risk and maximizing long-term success.
At Plaza Dental Parker, we take a personalized approach: every treatment plan begins with listening to your goals, evaluating clinical needs, and reviewing all available options. That ensures the chosen solution aligns with both your oral health requirements and your expectations for comfort and appearance.
The implant journey starts with planning—digital imaging, models, and a clear timeline for placement and restoration. The surgical step places the implant into the bone under controlled conditions; for many patients this is a well-managed, outpatient experience with options for local anesthesia or sedation if needed.
Following placement, a healing interval allows the implant to integrate with the bone. During this period you may wear a temporary restoration to maintain appearance and function. Once integration is confirmed, your clinician attaches the final prosthesis, carefully shaping and shading crowns or bridges to match your bite and smile for a natural result.
Some cases require additional procedures—such as sinus lifts or bone grafting—to build a secure foundation. These are common and predictable interventions that improve the long-term outcome of an implant-supported restoration.
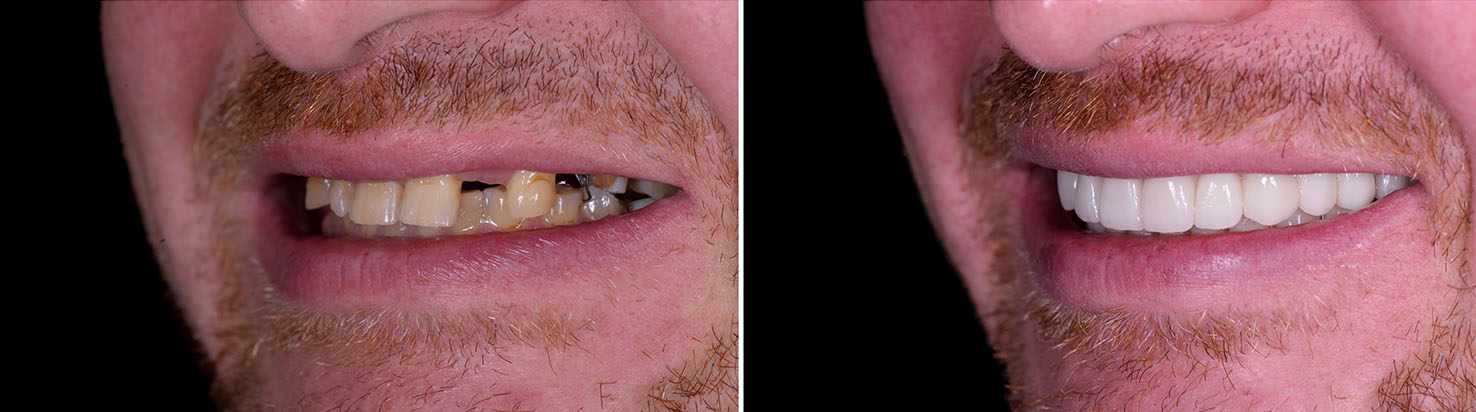
Bone grafting is a routine technique used to restore lost bone volume and create a stable site for implant placement. Bone can be augmented at the time of extraction, or grafted ahead of implant surgery when long-term bone loss has occurred. Grafting materials and techniques vary, but the goal is consistent: provide enough quality bone so the implant can integrate successfully.
Healing after grafting is monitored closely. Once the graft has matured and integrated, the implant placement proceeds according to the original treatment plan. With modern materials and careful planning, bone grafting frequently enables implant solutions that would otherwise be impossible, expanding options for patients who might have been told they were not candidates in the past.
Replacing missing teeth with implants is a collaborative process between you and your dental team. It starts with a conversation about your goals, an in-person evaluation, and a clear, personalized plan for moving forward. The result can be a stable, natural-looking smile that supports daily life and long-term oral health.
If you would like to learn whether dental implants are right for you, contact us for more information. Our team at Plaza Dental Parker is happy to answer your questions and guide you through the options available so you can make an informed decision about restoring your smile.
Dental implants are medical devices that replace a missing tooth by restoring both the root and the visible crown. A small titanium or zirconia post is surgically placed into the jawbone and, over time, the bone bonds to the implant in a process called osseointegration. This creates a stable anchor that supports a crown, bridge, or denture and replicates the function of a natural tooth root. The final restoration is shaped and shaded to match surrounding teeth so it integrates with your bite and appearance.
Implants are designed from biocompatible materials that resist corrosion and integrate with bone tissue to provide long-term stability. Because the implant transmits chewing forces into the jaw, it helps maintain bone volume and facial contours that can otherwise diminish after tooth loss. Implants do not decay like natural teeth, but the tissues around them require regular care to prevent inflammation. With appropriate planning and maintenance, implants can restore comfortable chewing, clear speech, and a natural-looking smile.
Candidacy for dental implants depends on a combination of oral and overall health factors rather than age alone. Clinicians evaluate the quantity and quality of jawbone, the health of the gums, and any medical conditions—such as uncontrolled diabetes or immune disorders—that could affect healing. Smoking and untreated periodontal disease can increase the risk of complications, so these factors are reviewed and managed as part of treatment planning. Imaging and a thorough clinical exam are essential to determine whether implant therapy is appropriate.
When bone volume is insufficient, many patients can still proceed with implants after bone grafting or sinus augmentation to rebuild the site. The treatment team will discuss how medical history, medications, and oral habits influence success and whether additional preparatory procedures are needed. An individualized plan takes all these variables into account so the chosen approach aligns with the patient’s functional and aesthetic goals at the outset.
Implant dentistry offers several restoration options that address single-tooth, multi-tooth, and full-arch needs. A single-tooth implant topped with a crown replaces an individual missing tooth without altering adjacent teeth, while implant-supported bridges replace multiple missing teeth by relying on implants for support. For patients missing all or most teeth, a full-arch fixed prosthesis can provide a permanent, non-removable restoration anchored by several implants.
Another common solution is an implant-retained overdenture, which uses implants to stabilize a removable denture and improve retention and comfort. The selection between single crowns, bridges, fixed full-arch prostheses, and overdentures depends on the number of missing teeth, bone availability, and patient preferences for removability and maintenance. Your clinician will explain the functional trade-offs and expected timeline for each option during planning.
The implant process begins with a comprehensive consultation that includes a medical and dental history review, clinical examination, and imaging such as CBCT or radiographs to assess bone anatomy. Based on that evaluation, the clinician creates a treatment plan that outlines implant positions, any preparatory procedures (for example, extractions or grafting), and the anticipated restorative approach. Planning often uses digital tools to improve precision and to coordinate surgical and prosthetic phases for predictable outcomes.
Surgery to place the implant is usually an outpatient procedure performed under local anesthesia or sedation, followed by a healing period to allow osseointegration. After the implant integrates with the bone, a second appointment involves attaching an abutment and fabricating the final crown, bridge, or denture. Some cases allow for immediate temporaries, but the timing of the final restoration is determined by bone quality, implant stability, and individual healing.
Bone grafting is a reconstructive procedure used when the jaw lacks sufficient bone volume or density to support an implant. Grafting materials can include the patient’s own bone, donor bone, or synthetic substitutes, and they serve as a scaffold to encourage new bone growth. Grafting may be performed at the time of tooth extraction, before implant placement, or simultaneously with implant surgery depending on the clinical situation and the surgeon’s assessment.
The success of a graft depends on proper technique, biological compatibility, and adequate healing time before implant placement when necessary. In many cases, grafting expands the number of patients who can receive implants by creating a stable foundation that supports osseointegration. Your dental team will explain the timeline and expected healing milestones so you understand how grafting fits into the overall treatment plan.
Implant surgery can be performed using several levels of anesthesia and sedation to match patient comfort and the complexity of the procedure. Local anesthesia numbs the surgical site and is commonly used for straightforward cases, while inhalation sedation (nitrous oxide), oral sedatives, or intravenous (IV) sedation can be offered for patients who prefer deeper relaxation. The choice depends on medical history, patient anxiety, procedural length, and practitioner training.
Before recommending a sedation option, the team reviews health history, current medications, and any previous reactions to sedatives or anesthesia to ensure safety. Monitoring during the procedure is standard practice to maintain stable vital signs, and patients receive clear pre- and post-operative instructions related to fasting, transportation, and recovery when sedation is used. Discussing preferences and concerns with the clinician helps determine the most appropriate approach.
Immediate recovery following implant placement typically involves some swelling, mild discomfort, and minor bleeding that peak within the first 48 to 72 hours and then gradually improve. Pain can usually be managed with prescribed or over-the-counter medications as advised by the clinician, and applying cold packs and resting help reduce swelling. Patients are often instructed to follow a soft diet for several days and to avoid strenuous activity to support healing at the surgical site.
The full process of osseointegration generally takes several weeks to several months depending on bone quality and implant location, and periodic follow-up visits monitor integration and soft tissue healing. Temporary restorations may be used to maintain appearance and function during this phase when appropriate. Clear post-operative care instructions and scheduled checkups ensure that healing proceeds predictably toward final restoration.
Long-term success of dental implants depends on daily oral hygiene and regular professional maintenance. Brushing twice a day with a low-abrasive toothpaste, cleaning around implants with interdental brushes or floss designed for implants, and rinsing as recommended help control plaque and reduce the risk of peri-implant inflammation. Smoking cessation and management of systemic conditions that affect healing are also important contributors to implant longevity.
Routine dental visits allow clinicians to assess soft tissue health, check occlusion, and take periodic radiographs to monitor bone levels around implants. If you grind your teeth, a night guard can protect both natural teeth and implant restorations from excessive forces. Promptly reporting any discomfort, mobility, or changes around an implant helps address issues early and supports durable outcomes.
While implants have a high success rate, potential risks and complications can include infection, peri-implantitis (inflammatory bone loss around the implant), implant failure or mobility, nerve injury, and sinus complications for implants placed in the upper jaw. Risk factors such as poor oral hygiene, untreated periodontal disease, smoking, and certain medical conditions can increase the likelihood of complications. Thorough evaluation and proper case selection reduce risk and help identify patients who may need additional preparatory treatment.
When complications occur, they are addressed through clinical interventions such as debridement, antibiotics, grafting, or implant removal and replacement when necessary. Regular follow-up and early intervention are key to managing problems effectively. Your dental team will explain specific risks related to your anatomy and medical history as part of informed consent and preoperative planning.
Getting started begins with a consultation that includes a review of your medical and dental history, a clinical exam, and imaging to evaluate bone and soft tissue. During this visit the team will discuss treatment goals, explain potential implant options, and outline a personalized care plan including any preparatory procedures that may be required. This initial planning step clarifies the anticipated timeline and the clinical steps needed to move forward safely.
If implants are a suitable option, subsequent appointments will focus on surgical placement, healing, and final restoration with close follow-up along the way. The office coordinates each phase so you understand what to expect at every visit and how to prepare for surgery and recovery. For residents of Parker, CO, scheduling a consultation is the first step toward exploring whether implants can restore function and appearance for missing teeth.
