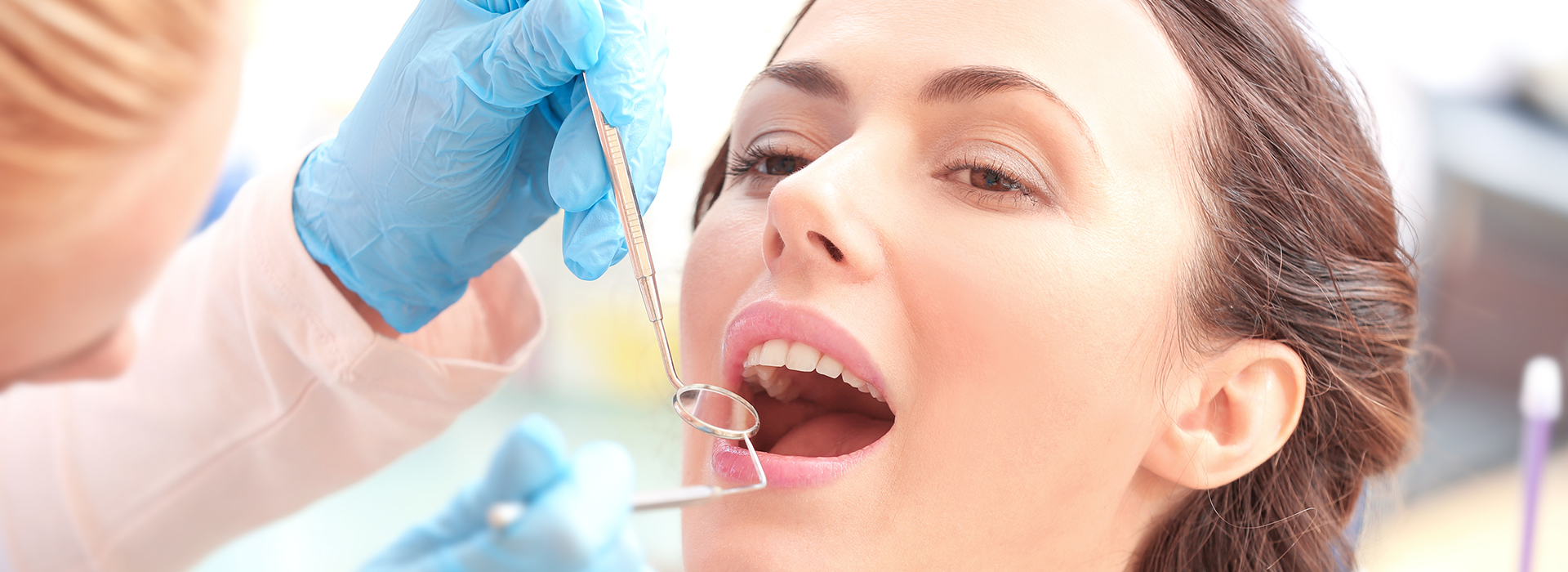
Gum disease is the leading cause of adult tooth loss, yet many people do not recognize its early signs. Research indicates that periodontal conditions affect a large portion of adults, but with timely care the course of the disease is often preventable. At Plaza Dental Parker, we focus on helping patients understand how gum disease develops and what practical, evidence-based steps can protect long-term oral health.
Healthy gums are the foundation of a stable, comfortable bite and a confident smile. The tissues that surround and support teeth — collectively called the periodontium — keep teeth anchored and protect the bone beneath. When inflammation from plaque and tartar persists, those supporting tissues respond with destruction rather than repair, and the consequences extend far past cosmetic concerns.
Because periodontal disease can progress without obvious pain, regular dental visits are crucial. During routine exams and hygiene appointments, clinicians look for subtle changes in gum color, texture, and pocket depth that indicate inflammation or tissue loss before problems become severe.
Understanding risk factors — such as tobacco use, uncontrolled diabetes, certain medications, and genetic predisposition — helps patients and clinicians work together to reduce vulnerability and keep periodontal conditions stable over time.
Common warning signs that warrant a dental checkup include:
Gums that appear swollen, red, or tender to the touch
Bleeding during brushing, flossing, or spontaneously
Gum recession exposing darker or sensitive tooth root surfaces
Sensitivity to temperature changes or certain foods
Persistent bad breath or an unpleasant taste in the mouth
Teeth that feel mobile or a change in how your bite fits together
New gaps forming between teeth or discomfort with dentures
Discharge or pus around the gums and soreness when chewing

Oral tissues are not isolated from the rest of the body. Chronic inflammation in the mouth can influence systemic health, and studies have shown associations between periodontal disease and conditions such as cardiovascular disease, stroke, diabetes management, and respiratory health. While these links are complex and still under study, reducing oral inflammation is an important component of general wellness.
Because of these connections, our clinical approach emphasizes prevention and early intervention. Simple measures taken now — improved daily hygiene, targeted professional cleanings, and monitoring by a dental professional — can lower the burden of oral bacteria and reduce inflammatory signals that may affect other organ systems.
When patients have medical conditions that influence healing or immune response, coordination with physicians can help shape a periodontal plan that is safe, effective, and tailored to individual health needs.
Gingivitis is the initial, reversible stage of gum disease. It is characterized primarily by redness, swelling, and bleeding caused by plaque buildup at the gumline. Importantly, gingivitis does not involve bone loss — that is what separates it from more destructive stages of periodontal disease.
Treatment at this stage focuses on removing the source of inflammation and supporting the tissues to recover. Professional hygiene visits combined with deliberate changes to home care usually restore gingival health. These interventions are most effective when started promptly, before the support structures of the teeth are compromised.
Patients often notice rapid improvements in tissue appearance and comfort after a short course of care, which reinforces the value of routine maintenance and consistent oral hygiene habits.

If gingivitis is not managed, the condition can progress to periodontitis, a stage where the connective tissues and bone that support teeth begin to break down. This process leads to deeper periodontal pockets, gum recession, and gradual bone loss. Over time, untreated periodontitis can compromise the stability of teeth and the overall function of the mouth.
Management at this stage aims to halt tissue destruction and preserve remaining support. That requires a careful assessment of pocket depths, bone levels, and the pattern of tissue loss so clinicians can design a targeted treatment plan that addresses infection and encourages healing.
When structural damage is present, modern periodontal therapy offers options to control disease activity and, in some cases, regenerate lost tissue to restore function and aesthetics.
Plaza Dental Parker provides a spectrum of periodontal services designed to match the severity and needs of each patient. Our clinicians combine mechanical cleaning, antimicrobial therapies, and when appropriate, surgical techniques to reduce bacterial burden, decrease pocket depth, and stabilize the periodontium.
Conservative measures are preferred when effective: improving oral hygiene, using targeted antimicrobials, and performing scaling and root planing can often stop progression without surgery. For cases that require more involved care, surgical procedures and regenerative approaches are considered to rebuild lost tissue and support.
Following active treatment, a structured maintenance program is essential. Regular periodontal maintenance visits reduce the risk of recurrence and help patients keep their gums healthy for the long term.
Selecting the appropriate periodontal therapy depends on clinical findings and the patient’s overall health. Factors such as pocket depth, amount of bone loss, bleeding on probing, and response to initial therapy guide the plan. A thorough examination and clear communication ensure patients understand the steps recommended and the goals of care.
When possible, treatment begins conservatively. Scaling and root planing — careful cleaning of root surfaces beneath the gumline — is a first-line approach to remove bacterial deposits and reduce inflammation. Adjunctive antimicrobials, localized delivery systems, or short courses of medication may be used selectively to enhance outcomes.
For early and many moderate cases of gum disease, non-surgical care is the most conservative and effective route. Scaling and root planing remove plaque and calculus beneath the gumline and smooth root surfaces to discourage bacterial recolonization.
Clinical outcomes improve when these procedures are paired with reinforced home care instruction and scheduled maintenance visits. Success depends on both professional intervention and the patient’s commitment to daily oral hygiene.
In some situations, localized antimicrobial therapy is placed directly into periodontal pockets to help reduce bacterial levels while tissues recover.
When pocket depths or tissue destruction exceed what can be managed conservatively, surgical options are considered. Procedures such as flap surgery allow clinicians to access root surfaces and underlying bone for thorough debridement and reshaping.
Regenerative procedures, including bone grafting and guided tissue regeneration, aim to rebuild lost bone and reattach soft tissue to the tooth root when conditions are favorable. These techniques can improve support, function, and the long-term prognosis of affected teeth.
Contemporary tools such as dental lasers are also used in select cases to reduce bacterial load, reshape soft tissue, and support healing. The choice of technique reflects the clinical situation and the patient’s goals for oral health and comfort.
If you have questions about signs of gum disease or would like to discuss periodontal care options, please contact us for more information.
Periodontal disease is an inflammatory condition that affects the gums and the supporting structures around the teeth, including the periodontal ligament and underlying bone. It begins when plaque bacteria at the gumline provoke an immune response that, if persistent, leads to tissue breakdown rather than repair. Early-stage gum inflammation, called gingivitis, is reversible with proper care, but untreated inflammation can progress to destructive periodontitis.
As the condition advances, pockets form between teeth and gums and bone can be lost, which compromises tooth stability and oral function. Multiple factors influence disease progression, including oral hygiene, smoking, systemic health, and genetic predisposition. Recognizing and addressing the condition early improves the likelihood of preserving natural teeth and restoring periodontal health.
Common warning signs that warrant an evaluation include gums that are swollen, red, or tender, bleeding during brushing or flossing, and persistent bad breath or an unpleasant taste. Patients may also notice gum recession exposing root surfaces, increased tooth sensitivity, or changes in how their bite feels. Mobility of teeth or new gaps forming between teeth are more advanced indications that deserve prompt attention.
Because periodontal disease can progress without severe pain, regular dental checkups and periodontal probing help detect subtle changes before irreversible damage occurs. If you observe any of these symptoms, contacting your dental provider for an assessment can allow for earlier, more conservative treatment. Early intervention typically leads to better outcomes and less invasive care.
Diagnosis relies on a thorough clinical exam that includes measuring pocket depths around teeth, assessing bleeding on probing, and evaluating gum recession and mobility. Dental radiographs are used to view bone levels and detect any loss of support that is not visible during the clinical exam. Together, these findings help categorize the disease stage and inform the treatment strategy.
A complete medical and dental history is also important because systemic conditions and medications can affect periodontal health and healing. Periodontal charting repeated over time demonstrates response to therapy and guides maintenance intervals. Clear communication between clinician and patient ensures the chosen plan reflects both clinical needs and the patient’s health status.
Non-surgical management typically begins with professional hygiene and scaling and root planing to remove plaque and calculus from beneath the gumline and smooth root surfaces. These procedures reduce bacterial burden and allow inflamed tissues to begin healing when combined with improved home care. In many early and moderate cases, conservative therapy is sufficient to halt progression and restore healthier gum tissue.
Adjunctive measures may include localized antimicrobial delivery into periodontal pockets, short courses of systemic medications when indicated, and tailored oral hygiene instruction to reinforce daily plaque control. Regular periodontal maintenance visits are essential after active therapy to monitor stability and prevent recurrence. Patient engagement with home care is a critical determinant of long-term success.
Surgical and regenerative interventions are considered when non-surgical therapy cannot adequately reduce pocket depths or when structural damage to bone and soft tissue threatens tooth support. Procedures such as flap surgery provide direct access for thorough debridement and allow clinicians to reshape bone and reposition tissue for improved health. Regenerative techniques, including bone grafting and guided tissue regeneration, aim to rebuild lost tissues when clinical conditions are favorable.
The decision to proceed with surgery is based on clinical measurements, radiographic findings, and the patient’s overall health and goals. Advances in materials and techniques have improved the predictability of regenerative care, but successful outcomes still depend on infection control and meticulous maintenance. Your clinician will review risks, benefits, and expected outcomes to determine the most appropriate approach.
Periodontal inflammation does not remain confined to the mouth; research has identified associations between chronic oral inflammation and systemic conditions such as cardiovascular disease, diabetes control, and respiratory health. While these links are complex and not fully causal in all cases, reducing oral bacterial load and inflammation is a modifiable factor that supports general wellness. Good periodontal care is therefore a component of comprehensive health management.
When patients have medical conditions that influence healing or immune response, coordination between dental clinicians and physicians helps ensure safe and effective periodontal care. Addressing periodontal disease can improve oral comfort and may contribute to better management of systemic conditions. Regular assessment and early intervention help minimize inflammatory burden and support whole-body health.
Scaling and root planing is a focused, non-surgical procedure in which clinicians remove plaque and calculus from tooth surfaces above and below the gumline and smooth rough root areas to discourage bacterial recolonization. Appointments may be completed quadrant by quadrant or in sections depending on clinical needs and patient comfort. Local anesthesia is often used to ensure a comfortable experience, and patients typically feel less tenderness as inflammation resolves.
After the procedure, clinicians will provide specific home care instructions and may recommend antimicrobial adjuncts or short-term medications when appropriate. Healing typically progresses over several weeks, during which follow-up visits assess tissue response and pocket depth reduction. Maintenance appointments are scheduled to monitor progress and prevent recurrence.
Antimicrobial therapies can be applied locally into periodontal pockets or, in selected cases, delivered systemically to reduce pathogenic bacteria and support healing after mechanical debridement. Localized delivery allows higher concentrations at the site of infection with minimal systemic exposure, and clinicians select agents based on specific clinical indications. These therapies are adjuncts to, not substitutes for, thorough mechanical cleaning.
Dental lasers are another adjunctive tool used in select situations to reduce bacterial load, remove diseased soft tissue, and promote coagulation and healing. Laser use depends on the clinical scenario and the clinician’s training and judgment, and outcomes are optimized when lasers are integrated with conventional therapies. Treatment planning always focuses on evidence-based approaches tailored to the patient’s needs.
Daily plaque control through proper brushing, interdental cleaning, and antiseptic rinses when appropriate is foundational to preventing and managing gum disease. Effective home care removes the biofilm that drives inflammation and enhances the long-term benefits of professional treatments. Patient education and habit reinforcement during hygiene visits are key components of a successful periodontal program.
Consistent oral hygiene is also essential after active therapy to maintain pocket depth reduction and tissue stability. Periodontal maintenance visits at clinician-recommended intervals enable early detection of recurrence and timely retreatment if necessary. Collaboration between patients and dental professionals yields the best outcomes for preserving periodontal health.
Treatment planning begins with a comprehensive evaluation of clinical measurements, radiographs, medical history, and risk factors such as smoking and diabetes that influence healing and disease progression. Clinicians prioritize conservative approaches when effective, starting with scaling and root planing and adding adjunctive therapies or surgical options only as needed to control infection and restore support. The patient’s goals, comfort, and overall health are incorporated into the decision-making process.
At Plaza Dental Parker, clinicians emphasize clear communication and shared decision making so patients understand the rationale for recommended steps and the importance of follow-up care. A structured maintenance schedule is established after active therapy to monitor stability and reduce the likelihood of recurrence. This individualized, evidence-based approach helps preserve oral function and long-term periodontal health.
