Temporomandibular joint (TMJ) disorders affect a wide range of people and can interfere with everyday activities like eating, speaking, and sleeping. These conditions involve the complex joints and muscles that control jaw movement, and their symptoms can be subtle or strikingly disruptive. Understanding how TMJ disorders develop, how they are evaluated, and which treatment paths are appropriate helps patients make informed choices about care and recovery.
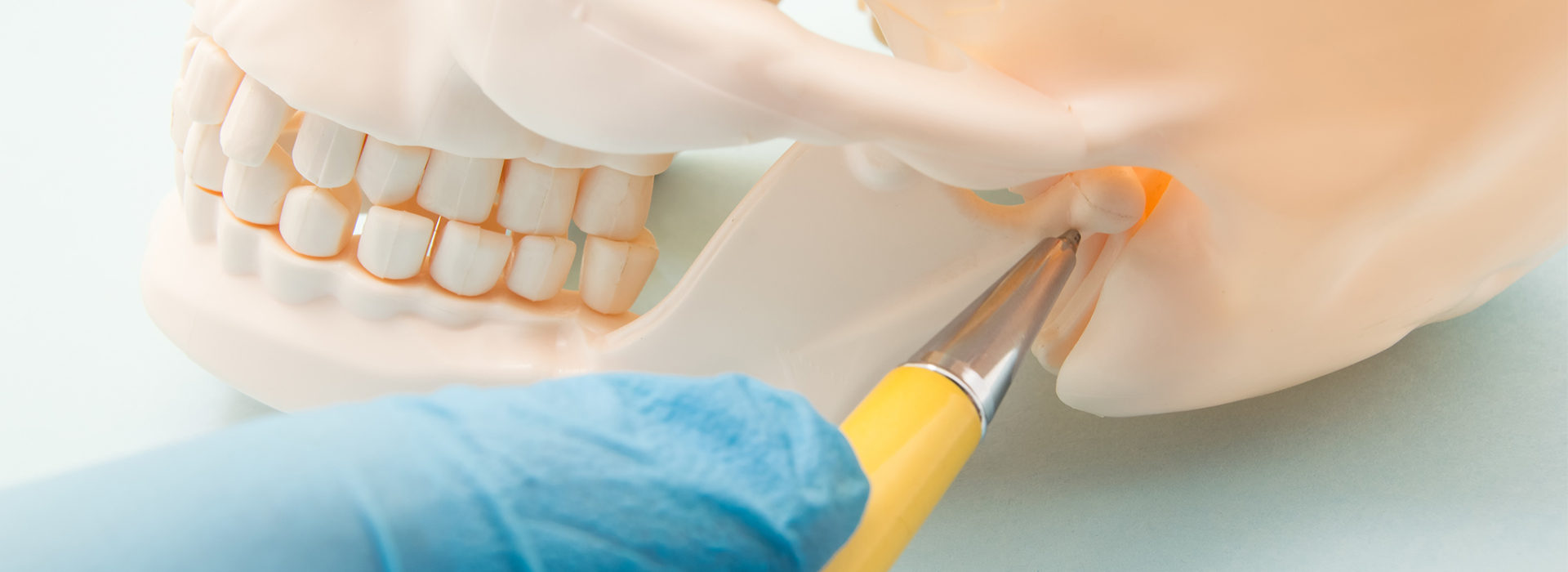
The temporomandibular joints connect the lower jaw (mandible) to the temporal bones of the skull on both sides of the head. Each joint contains a small, cushioning disc, a rounded condyle on the mandible, and an intricate network of ligaments and muscles that coordinate movement. Together these structures allow the jaw to hinge, glide, and rotate, enabling a surprisingly wide range of motions for speaking, chewing, yawning, and facial expression.
Because the TMJ must accommodate both hinge-like and sliding motions, it is mechanically more complex than many other joints. That complexity makes the joint vulnerable to several different types of stress and injury. When the balance among muscles, teeth, joint surfaces, and the disc is disrupted, even routine movements can become painful or restricted.
Recognizing the TMJ’s role in everyday function is the first step in understanding why symptoms can vary so much from person to person. Some patients experience intermittent clicking without pain, while others face persistent discomfort, limited opening, or frequent jaw locking that affects quality of life.
TMJ disorders have many contributing factors rather than a single cause. Repetitive strain from clenching or grinding the teeth (bruxism) is one of the most common triggers because it increases pressure on the joint and surrounding muscles. Acute trauma — such as a jaw injury or a blow to the face — can also lead to joint dysfunction or disc displacement.
Systemic conditions play a role as well. Degenerative joint disease like osteoarthritis and inflammatory conditions such as rheumatoid arthritis can affect the TMJ, altering joint surfaces and causing pain or limited movement. In other cases, changes in bite alignment, missing teeth, or dental work that affects how the teeth come together can contribute to abnormal forces on the joint.
Psychological factors matter, too: chronic stress and anxiety often manifest as increased jaw tension and muscle tightness. Age and gender patterns are observable in clinical practice, with certain cohorts reporting TMJ symptoms more frequently, but the disorder can occur at any age and in anyone who experiences prolonged joint or muscle strain.
TMJ disorder symptoms range broadly. Common complaints include jaw pain or aching around the ear, tenderness of the muscles that control chewing, and noticeable popping, clicking, or grating sounds when opening or closing the mouth. For some people these sounds are harmless; for others they accompany pain or a feeling that the jaw is “out of place.”
Many patients also experience restricted jaw motion — difficulty opening wide, or episodes where the jaw becomes temporarily stuck in an open or closed position. Associated symptoms may extend beyond the jaw, including headaches, neck or shoulder pain, ear fullness, and sensitivity that resembles an earache or sinus pressure. These overlapping signs can make diagnosis challenging without a careful exam.
Because symptoms can mimic other conditions, it’s important for patients to describe when problems started, what activities make symptoms better or worse, and whether any recent injuries or dental changes coincided with the onset. A clear symptom history helps guide a focused clinical evaluation and a tailored plan of care.
An accurate assessment begins with a comprehensive clinical exam. The dentist evaluates jaw range of motion, listens for joint sounds, palpates muscles for tenderness or spasm, and observes how the teeth fit together. This hands-on evaluation helps differentiate muscular pain from internal joint problems and identifies functional limits that affect daily life.
Imaging is used selectively to clarify structural issues. Panoramic X-rays, cone beam CT scans, or MRI studies may be recommended when there is concern about disc displacement, degenerative changes, or suspected joint injury. These tools provide detailed information about bone structure and soft tissues that cannot be determined by a physical exam alone.
A thorough diagnosis often combines clinical findings, imaging results, and a review of contributing factors such as parafunctional habits, medical history, and prior dental treatments. When necessary, the dental team coordinates care with other professionals — for example, physical therapists, otolaryngologists, or pain specialists — to ensure a multidisciplinary approach to complex or persistent cases.
At our practice in Parker, CO, we focus on careful evaluation and clear communication, so patients understand the nature of their condition and the rationale behind recommended next steps. This collaborative process sets realistic expectations and helps patients take an active role in their recovery.
Most treatment plans begin with conservative, reversible measures designed to reduce pain and restore function. Behavior changes — such as avoiding hard foods, limiting wide yawns, and reducing nail- or pencil-biting — can relieve strain. Simple at-home strategies like applying warm compresses, practicing gentle jaw stretching, and using relaxation techniques often ease muscle tension.
Dental interventions commonly include custom-fitted oral appliances, such as night guards or stabilization splints, which protect teeth from grinding and help reduce harmful joint loading. Physical therapy focused on posture, joint mobilization, and targeted muscle exercises can improve coordination and reduce pain. Short courses of medication may be prescribed for pain control or to relax overactive muscles, always with attention to safety and suitability for the individual patient.
When noninvasive approaches do not provide sufficient relief, minimally invasive procedures such as joint injections or arthrocentesis may be considered to address intra-articular inflammation or adhesions. Surgical options are reserved for specific, well-defined structural problems that do not respond to other therapies; these procedures require careful evaluation and are performed selectively with the goal of improving function and reducing long-term symptoms.
Throughout treatment, the emphasis is on individualized care that balances symptom relief with preservation of joint health. Many patients achieve meaningful improvement without surgery, and ongoing follow-up helps ensure adjustments are made as needs change over time.
In summary, TMJ disorders encompass a variety of conditions that affect the jaw’s joints and muscles and can significantly impact daily comfort and function. With a thoughtful diagnostic process and a range of conservative and advanced treatment strategies, patients can often reclaim normal function and reduce pain. If you have concerns about jaw pain, clicking, or limited movement, please contact us to learn more about how we evaluate and manage TMJ disorders.
TMJ disorders arise from a variety of factors that affect the joints, muscles, and surrounding structures that control jaw movement. Common contributors include repetitive strain from clenching or grinding the teeth (bruxism), acute trauma to the jaw, and changes in bite alignment that alter how the teeth come together. Systemic conditions such as osteoarthritis or inflammatory arthritis can also affect the joint surface and its cushioning disc, increasing the risk of dysfunction.
Psychological and behavioral factors play a role as well; chronic stress and anxiety often lead to increased muscle tension and parafunctional habits that burden the joint. Dental treatments or missing teeth that change the way the bite meets can create abnormal loading on the TMJ over time. Because TMJ disorders usually result from multiple interacting causes, a careful evaluation is important to identify the dominant contributing factors for each patient.
Symptoms of TMJ disorders vary widely but commonly include jaw pain or aching around the ear, tenderness in the chewing muscles, and noises such as popping, clicking, or grating when opening or closing the mouth. Some people experience restricted jaw motion, difficulty opening wide, or episodes of the jaw locking open or closed, which can significantly interfere with eating and speaking. Many patients also report associated symptoms such as headaches, ear fullness, neck or shoulder discomfort, and sensitivity that can feel like an earache or sinus pressure.
Because these signs overlap with other conditions, it is important to note symptom patterns — when pain began, activities that worsen or relieve it, and any recent injuries or dental changes. Intermittent clicking without pain may be observed in otherwise healthy individuals, while persistent pain or functional limits warrant a focused clinical evaluation. A clear symptom history helps the dental team determine the likely source of the problem and plan appropriate next steps.
An accurate diagnosis begins with a comprehensive clinical exam that assesses jaw range of motion, listens for joint sounds, palpates muscles for tenderness or spasm, and examines how the teeth come together. The clinician will review the patient’s medical and dental history, ask about parafunctional habits like grinding, and observe functional patterns that suggest muscular versus joint-based pain. These hands-on findings often guide the selection of imaging or referrals when structural concerns are suspected.
Imaging is used selectively to clarify intra-articular conditions or bony changes and may include panoramic X-rays, cone beam CT, or MRI for soft-tissue evaluation when disc displacement is a concern. Diagnostic information is integrated with the clinical exam to distinguish muscular pain from internal joint pathology and to identify any contributing dental or systemic factors. When cases are complex, the dental team may coordinate with physical therapists, ENT specialists, or pain management professionals to ensure a multidisciplinary approach.
Most TMJ treatment programs start with conservative, reversible measures aimed at reducing pain and restoring function. Recommendations typically include behavior modification such as avoiding hard or chewy foods, limiting wide yawns, and reducing habits like nail-biting or pencil-chewing, combined with at-home care like warm compresses, gentle stretching, and relaxation techniques to ease muscle tension. Short courses of medication to manage pain or reduce muscle spasm may be appropriate in selected cases, always tailored to individual medical history and safety considerations.
Dental appliances, such as custom-fitted night guards or stabilization splints, are commonly used to protect teeth from grinding and to redistribute forces on the joint and muscles. Physical therapy that emphasizes posture, targeted exercises, and soft-tissue mobilization can improve coordination and reduce pain for many patients. Regular follow-up allows the clinician to adjust conservative strategies and monitor progress before considering more invasive interventions.
Minimally invasive procedures like corticosteroid or hyaluronic acid injections and arthrocentesis (joint lavage) are considered when conservative care fails to provide adequate relief and there is evidence of intra-articular inflammation or adhesions. These interventions aim to reduce pain, decrease inflammation, and improve joint mobility while avoiding the higher risks associated with open surgery. The decision to proceed with injections is guided by clinical findings, imaging results, and a clear discussion of expected benefits and limitations.
Surgical options are reserved for well-defined structural problems — such as severe degenerative changes, persistent disc displacement unresponsive to other therapies, or mechanical impediments to normal function — and are recommended only after thorough evaluation and consideration of noninvasive alternatives. When surgery is being contemplated, care is coordinated with oral and maxillofacial surgeons or other specialists to ensure appropriate planning and postoperative rehabilitation. The overall goal is to improve function and quality of life while minimizing long-term risks to the joint.
Custom-fitted oral appliances, including stabilization splints and night guards, are designed to protect teeth from grinding and to reduce excessive loading on the TMJ and associated muscles. By creating a more even distribution of bite forces and preventing harmful clenching patterns during sleep, these devices often decrease muscle overactivity and allow inflamed tissues to recover. Properly fabricated appliances are tailored to each patient’s bite and should be adjusted by the treating dentist to ensure comfort and effectiveness.
While appliances can provide significant symptom relief for many patients, they are typically part of a broader treatment plan that includes behavior modification and, when appropriate, physical therapy or stress management. Regular monitoring is important to assess appliance fit and function over time and to make adjustments as the patient’s symptoms change. Long-term success usually depends on addressing underlying contributing factors in addition to using a protective device.
Effective self-care strategies include avoiding hard, chewy, or sticky foods; practicing gentle jaw stretches; and applying warm compresses to relieve muscle tension. Relaxation techniques such as diaphragmatic breathing, progressive muscle relaxation, or biofeedback can reduce overall muscle tension and lower the frequency of clenching episodes that exacerbate TMJ pain. Maintaining good posture, especially during long periods of computer work or phone use, helps decrease strain on the neck and jaw muscles.
Keeping a symptom diary can help identify patterns and triggers, such as particular activities or stressors that worsen pain, which supports more targeted behavioral changes. Over-the-counter pain relievers may provide short-term relief for some patients, but they should be used judiciously and in consultation with a healthcare provider when needed. If home measures do not lead to improvement within a few weeks or if function is noticeably limited, seek evaluation by your dental team for a tailored treatment plan.
You should seek an evaluation if jaw pain persists beyond a few weeks, if you notice progressive difficulty opening or closing your mouth, or if joint noises are accompanied by pain or locking that interferes with daily activities. Early assessment helps distinguish temporary muscular pain from conditions that may require more focused intervention or imaging. Timely care can prevent worsening symptoms and improve the chances of responding well to conservative therapy.
If jaw pain follows facial trauma, or if you experience sudden changes in bite, numbness, or severe swelling, prompt attention is especially important to rule out acute injury or other urgent problems. For ongoing concerns, the team at Plaza Dental Parker in Parker, CO, can perform a thorough examination and coordinate multidisciplinary care when necessary to address complex or persistent cases. A clear treatment plan and regular follow-up support better outcomes and help restore comfortable function.
Bruxism, or teeth grinding and clenching, commonly occurs during sleep and places repetitive stress on the temporomandibular joints and surrounding muscles, often contributing to the development or exacerbation of TMJ symptoms. Sleep-related bruxism can cause morning jaw pain, tooth sensitivity, and increased joint noise, and over time it may lead to muscle fatigue and joint inflammation. Identifying whether grinding occurs during sleep often involves patient history, partner reports, and clinical signs such as tooth wear and muscle tenderness.
Because sleep-disordered breathing and sleep quality can influence bruxism and muscle tension, a comprehensive evaluation sometimes includes discussion of sleep habits and screening for obstructive sleep apnea when relevant. Management strategies may combine oral appliance therapy, behavioral changes, and referral to sleep specialists if needed. Coordination among dental, medical, and sleep care providers can improve both sleep-related issues and TMJ symptom control.
Children and adolescents can develop TMJ symptoms, often related to habits like chewing nonfood items, nail-biting, or nighttime grinding, as well as orthodontic changes that affect how the teeth meet. Growth-related changes in the jaw and bite may influence joint mechanics, and clinicians carefully evaluate whether symptoms are transient during development or indicate a more persistent problem. Because younger patients are still growing, treatment emphasizes conservative, reversible measures whenever possible.
Initial management for pediatric patients typically includes behavior modification, simple home care, and monitoring, with custom appliances considered only when clearly indicated and appropriately sized for the child. Coordination with orthodontists, pediatric dentists, or pediatricians helps ensure that growth and dental development are considered in any treatment plan. Early education about habits, posture, and stress management often reduces symptoms and supports long-term joint health.
